新产程管理模式下活跃期不同时限对母婴结局的影响
崔建玲 廖晓礼 曾丽香


[摘要]目的 探討新产程管理模式下活跃期不同时限对母婴结局的影响。方法 回顾性分析2018年7月~2019年7月我院妇产科收治的360例足月初产妇的临床资料,根据活跃期的不同进行分组,将其中180例活跃期<4 h的产妇纳入对照组,将另外180例活跃期≥4 h的产妇纳入观察组。比较两组产妇围术期指标、新生儿分娩后1、5 min Apgar评分、妊娠结局以及妊娠并发症发生情况。结果 观察组产妇产后出血量少于对照组,总产程时间长于对照组,差异有统计学意义(P<0.05);两组新生儿分娩后5 min的Apgar评分与分娩后1 min比较,差异无统计学意义(P>0.05);观察组产妇中转剖宫产率低于对照组,差异有统计学意义(P<0.05);两组羊水粪染及新生儿窒息发生率比较,差异无统计学意义(P>0.05)。结论 新产程管理模式以活跃期停滞时间>4 h再考虑是否作为手术的指征,可使产妇有充分的时间试产,降低剖宫产率,改善围术期指标,利于产妇预后,推荐临床推广应用。
[关键词]新产程管理模式;活跃期不同时限;母婴结局
[中图分类号] R714 [文献标识码] A [文章编号] 1674-4721(2020)7(b)-0122-03
Effect of different time limits of active period on maternal and infant outcomes under the new labor management mode
CUI Jian-ling1 LIAO Xiao-li1 ZENG Li-xiang2
1. Department of Obstetrics, Medical and Child Health Care and Family Planning Service Center of Huizhou City, Guangdong Province, Huizhou 516001, China; 2. Department of Medical Records, Medical and Child Health Care and Family Planning Service Center of Huizhou City, Guangdong Province, Huizhou 516001, China
[Abstract] Objective To explore the effect of different time limits of active period on the maternal and infant outcomes under the new labor management model. Methods Retrospective analysis of the clinical data of 360 full-term primiparas treated to the department of obstetrics and gynecology in our hospital from July 2018 to July 2019. Grouped according to the different active periods, 180 pregnant women with active period <4 h were included in the control group, and another 180 pregnant women with active period ≥4 h were included in the observation group. The perioperative indicators, the Apgar scores at 1 minute and 5 minutes after delivery, the pregnancy outcomes and complications were compared between the two groups. Results The maternal postpartum hemorrhage volume in the observation group was lower than that in the control group, and the total duration of labor was longer than that in the control group, the differences were statistically significant (P<0.05). There were no significant differences in the Apgar score of newborns between the two groups 5 minutes after delivery and 1 minute after delivery (P>0.05). The rate of maternal conversion tocesarean section in the observation group was lower than that in the control group, and the difference was statistically significant (P<0.05). There was no significant difference in the incidence of amniotic fluid fecal infection and neonatal asphyxia between the two groups (P>0.05). Conclusion The new labor management mode takes the active period >4 h as the treatment time limit to allow the pregnant women to have sufficient time for trial delivery, reduce the cesarean delivery rate, improve the perioperative index, and benefit the prognosis of the pregnant women. It is recommended of clinical application.
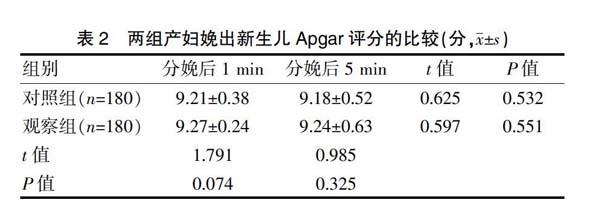
为此本研究将新产程管理模式应用于产妇分娩,观察其不同活跃期时限对于两组产妇的围术期指标、新生儿分娩后1、5 min的Apgar评分以及妊娠结局与妊娠并发症发生情况的差异。结果显示,观察组产妇产后出血量少于对照组,中转剖宫产率低于对照组,总产程时间长于对照组,差异有统计学意义(P<0.05);两组新生儿分娩后5 min的Apgar评分与分娩后1 min的评分、羊水粪染及新生儿窒息发生率比较,差异无统计学意义(P>0.05)。提示新产程管理模式利于改善产妇围术期指标,且将活跃期>4 h不进展作为活跃期停滞标准时,产妇转行剖宫产率更低,但对于新生儿评分及并发症无明显意义。究其原因在于,新产程管理模式相较于Friedman产程图而言,其以宫口擴张至6 cm作为活跃期起点,以4 h不进展作为活跃期停滞,要积极寻找原因,将产程时间与活跃期时间充分延长,可显著降低转剖宫产率,同时也使产妇有充足的阴道试产时间[12-13]。此外,活跃期停止进展时间>4 h时,可减少分娩产程中的医疗干预,使初产妇分娩过程遵循自然规律,顺利经阴道分娩[14-16]。
综上所述,初产妇采用新产程管理模式有利于改善围术期指标,且将活跃期>4 h不进展诊断为活跃期停滞标准可显著降低剖宫产率,促进自然分娩,值得临床应用推广。
[参考文献]
[1]钱夏柳,詹泽森,覃惠凤.以新产程标准为指导的产程处理对分娩结局的影响研究[J].中国全科医学,2017,20(15):1845-1848.
[2]赵娜,李娜,蒋小芒,等.新产程标准对产程中临床指征及母婴预后的影响[J].现代生物医学进展,2017,17(27):5362-5364.
[3]谌雯丽,秦丰江,吴庆蓉,等.新产程标准管理下无痛分娩对妊娠结局的影响[J].浙江临床医学,2019,21(8):1057-1058.
[4]时春艳,李博雅.新产程标准及处理的专家共识(2014)[J].中华妇产科杂志,2014,23(7):486.
[5]李容芳,徐燕媚,邓琼.新产程标准中活跃期拐点在初产妇与经产妇临床应用中的影响[J].热带医学杂志,2017, 17(7):932-935.
[6]姜丽,曹云桂,张青.持续性剖宫产瘢痕妊娠的临床特点分析[J].中国计划生育学杂志,2019,27(1):99-101.
[7]周友芬,郭雅琴,邓艳华,等.新产程图产程管理在初产妇中的应用效果[J].中国妇幼保健,2018,33(5):994-996.
[8]孟璐璐,苏秀娟,花静,等.产程图的研究历程[J].中华围产医学杂志,2018,21(11):780-782.
[9]黄秋明,陈晖,梁美娟,等.新产程标准的应用对妊娠结局的影响[J].海南医学,2017,28(6):989-990.
[10]包菊,赫英东,包艾荣,等.新产程标准下全产程分娩镇痛对母婴结局的影响[J].中华围产医学杂志,2019,22(2):106-112.
[11]杨小妹,冯小明,张蕾,等.阴道分娩过程中新产程时限管理标准的临床效果[J].中国妇幼保健,2018,33(7):1504-1506.
[12]叶立.以产程特性比较为基础的新旧产程标准临床实践效果研究[J].检验医学与临床,2017,14(13):1951-1953.
[13]马瑶,陈磊,曹冬如,等.实施新产程及催引产指南后剖宫产率及剖宫产指征的变化分析[J].中国生育健康杂志,2017,25(5):468-469,478.
[14]王春芳,王慧敏,欧阳林.新产程标准与助产措施对产钳助产、中转剖宫产和新生儿窒息发生率的影响分析[J].医学临床研究,2017,34(6):1135-1137.
[15]陆眸清,冯碧波,翟建军,等.新产程实施对助产、中转剖宫产及母儿结局的影响[J].中国医药导报,2018,15(21):90-93.
[16]刘兰,王金莲,张立敏,等.新产程标准下剖宫产后阴道试产239例妊娠结局[J].安徽医药,2019,23(5):939-941.
(收稿日期:2019-12-18)

